
California Governor Gavin Newsum cleared his desk and took his final legislative action in October for the 2023 year, which included signing Health Care Bill AB 1070 into law.

This legislation would grant permission for a physician and surgeon to oversee a maximum of eight physician assistants concurrently, provided that all the physician assistants are exclusively dedicated to conducting in-home health assessments to collect patient data and conduct annual wellness check-ups or health evaluations that do not entail direct patient treatment or medication prescription. Previously, the law prohibited physicians and surgeons in California from overseeing more than four PAs simultaneously.
These evaluations encompass comprehensive physical examinations, health conditions and social determinants of health assessments, medication reviews, screening tests, and health education.
The exemption is unique to California and will go into action on January 1, 2024. The legislation applies to PAs focused on conducting health evaluations corresponding to Medicare’s “annual wellness visits.”
The Birth of the Physician Assistant: A New Role for Ex- Military Corpsmen
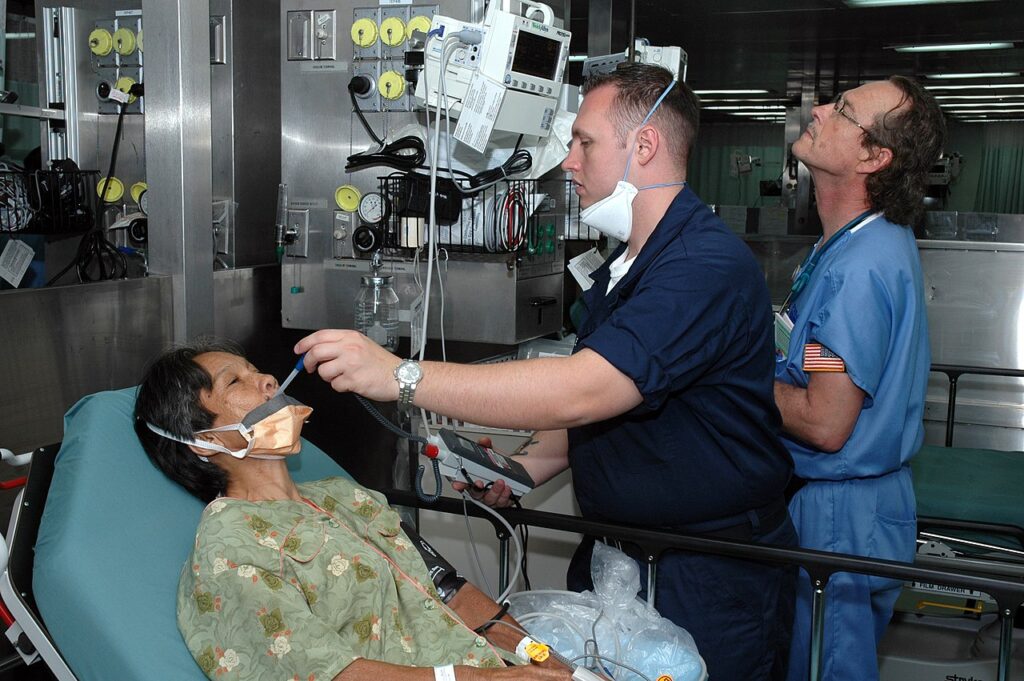
The PA role started as a ‘suggestion‘ offered by Dr. Charles Hudson in 1961 at a conference on medical education hosted by the American Medical Association. An internal medicine doctor, Dr. Hudson, recommended ‘assistants to doctors’ to offset the growing healthcare gap. He proposed ex-medical corpsmen as the perfect candidates because they were highly trained with little to no opportunity to practice their skills once they left the military and returned home. The first PA program took place at Duke University as a two-year program in 1965. The first three graduating students graduated on October 6, 1967.
The Impact of Physician Assistants in Healthcare
The PA role is experiencing a rapid growth spurt in the United States. The National Commission Board on Certification of Physician Assistants reported 168,318 PAs at the end of 2022. Mississippi, South Carolina, and Indiana experienced the highest percentage of growth of board-certified PAs from 2018 to 2022.
According to various research studies, employed PAs are expected to grow 31.3 % by 2029. PAs are competent associates in the ever-evolving healthcare delivery system landscape. Due to the current physician shortage, PAs are filling in the provider gaps.
Common Places PA’s are Employed
- Hospitals: Many PAs work in various departments, including emergency rooms, surgery, internal medicine, pediatrics, etc. They assist in patient care, perform procedures, and collaborate with physicians and other healthcare providers.
- Physician Offices/Clinics: PAs often work in outpatient settings, providing primary care, specialty care, and preventive services. They can be found in family medicine, cardiology, dermatology, and many other specialties.
- Urgent Care Centers: Urgent care facilities employ PAs to provide immediate, non-emergency healthcare services. They diagnose and treat a wide range of illnesses and injuries.
- Community Health Centers: PAs play a significant role in community health centers providing primary care services to underserved populations. They address the healthcare needs of diverse communities.
- Surgical Settings: Some PAs specialize in surgical procedures and work closely with surgeons in the operating room. They may assist in surgeries, conduct pre-operative and post-operative care, and provide surgical consultations.
- Long-Term Care Facilities: PAs can care for elderly and chronically ill patients in nursing homes, assisted living facilities, and rehabilitation centers.
- Mental Health Settings: In mental health and psychiatry, PAs work alongside psychiatrists to diagnose and manage mental health conditions, prescribe medications, and provide therapy.
- Rural and Underserved Areas: PAs are often deployed to rural and underserved regions with a shortage of healthcare providers. They help bridge the gap in healthcare access.
- Education and Research: Some PAs work in academic and research institutions, where they may be involved in training future PAs, conducting clinical research, or developing healthcare policies.
- Government and Military: PAs can serve in various government agencies, such as the Department of Veterans Affairs or the military, providing healthcare to veterans and active-duty personnel.
- Corporate Health: Some large companies employ PAs to oversee employee health and wellness programs, conduct physical exams, and provide healthcare services to their staff.
- Telemedicine: With the growth of telehealth, PAs are increasingly offering virtual healthcare services, diagnosing and treating patients remotely via video consultations.
It’s important to note that PAs specific roles and responsibilities may vary depending on the setting and state regulations. PAs can adapt to different healthcare environments and contribute significantly to improving patient care and healthcare access.
Roles and Responsibilities
- Patient Care: PAs are trained to perform thorough medical evaluations, order and interpret diagnostic tests, and diagnose and manage various medical conditions. They can also provide preventive care, such as vaccinations, health screenings, and counseling.
- Treatment Planning: Physician assistants work closely with physicians to develop and implement patient treatment plans. This may involve prescribing medication, recommending therapies, and making necessary referrals to specialists.
- Procedures: In some cases, PAs can perform medical procedures, like suturing wounds, setting fractures, and assisting in surgery. This helps in ensuring that patients receive prompt and effective care.
- Education and Counseling: PAs often educate patients about their conditions, treatment options, and ways to maintain good health. They provide valuable information to help patients make informed decisions about their healthcare.

Physician assistants are instrumental in improving healthcare accessibility and quality. Here’s how they make a difference:
- Meeting Growing Healthcare Demands: PAs help alleviate the physician shortage and extend the reach of healthcare services to underserved communities.
- Cost-Effective Care: They offer cost-effective healthcare, reducing the burden on patients and the healthcare system.
- Enhanced Patient Experience: PAs often spend more time with patients, offering a more personalized and empathetic approach to care.
- Team-Based Care: They work collaboratively with physicians, nurses, and other healthcare professionals, creating a more comprehensive and efficient approach to patient care.
Education and Training
- Bachelor’s Degree: PAs usually start with a bachelor’s degree in a healthcare-related field, which includes prerequisite coursework in biology, chemistry, and other science subjects.
- Master’s Degree: They then enroll in a Master of Physician Assistant Studies (MPAS) program, which typically takes two years to complete. These programs include both classroom instruction and clinical rotations.
- Certification: After graduation, aspiring PAs must pass the Physician Assistant National Certifying Examination (PANCE) to become certified PAs. This certification is required in all states.
- Licensure: PAs must also obtain a state license to practice, which may include passing a state-specific exam.
